Dooley Noted: 5/16/16
My patient told me today that she went to the ER after having ribside pain that she suspected might be organ referral.
Luckily, she was cleared of any organ involvement and released to her therapists to handle a muscular pull.
When she expressed that she may have jumped the gun coming to emergency, the ER doctor congratulated her for doing the right thing.
He said, “I’ve literally seen patients die of embarrassment.”
People can choose to avoid their discomforts, assuming they will dissipate.
And that’s okay – if they do indeed pass.
A muscle spasm can be perceived as painfully as an arterial rupture.
Pain, after all, is subjective.
Pain is an alarm that something is awry, even if the problem isn’t serious.
There’s no need to be embarrassed of your discomforts.
But since many organ referrals can masquerade as muscle pain, consider these truths:
1. Heart issues can mimic chest tightness and left shoulder, jaw, and arm pain.
2. Gall bladder dysfunction can mimic right shoulder blade and upper shoulder referral pain, radiating to the ribcage.
3. Pancreatitis and aortic aneurysms can create a sole symptom of low back dull and relentless pain.
4. Cerebral tumors and arterial issues can cause headaches and/or eye pain and changes in vision.
5. Ovarian cysts and uterine fibroids can create anterior hip pain and abdominal bloating.
6. Kidney issues can cause flank pain or mid-to low-back pain, where ribs meet the vertebrae.
7. Urinary bladder or rectal issues may present with pelvic floor downward-bearing pressure or tailbone pain.
8. Intestinal issues can show as peri-umbilical pain, low back pain, or flank pain.
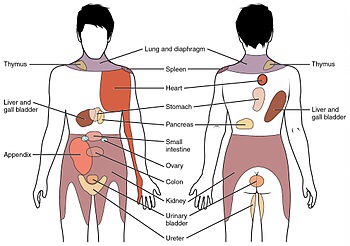
These are just a few of the most common patterns of organ referral pain mimicking musculoskeletal pain.
To rule out systemic issues of organ referral patterns, always see a qualified therapist who takes a solid history.
Since the skin and musculature are innervated by the same nerves that supply the body wall lining of the thorax and abdomen, many organ referrals can show up as musculoskeletal symptoms.
Always be better safe than sorry.
Get assessed and corrected.
No one needs to die of embarrassment.
As always, it’s your call.
– Dr. Kathy Dooley
